Root canal treatment is a dental procedure that removes the infected or damaged pulp from the inside of a tooth. The pulp is the soft tissue that contains neurons and blood vessels.
When the pulp becomes infected, it can cause discomfort, swelling, and abscesses. Root canal therapy can save a tooth that would otherwise have to be extracted.
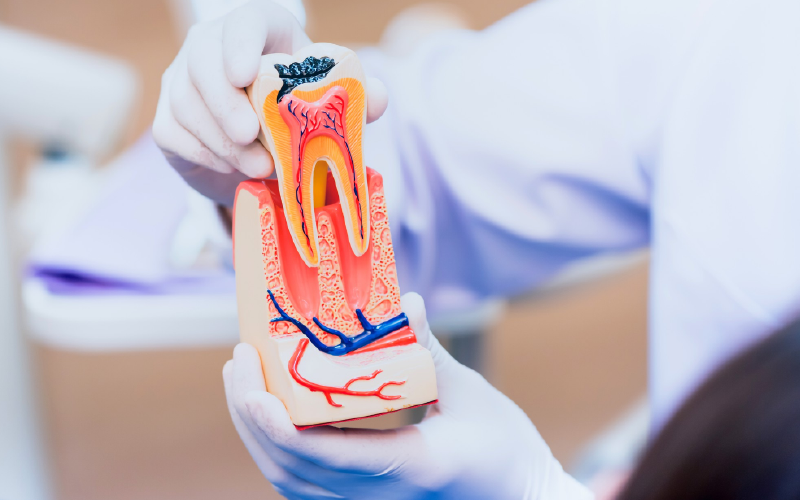
What is Dental Pulp?
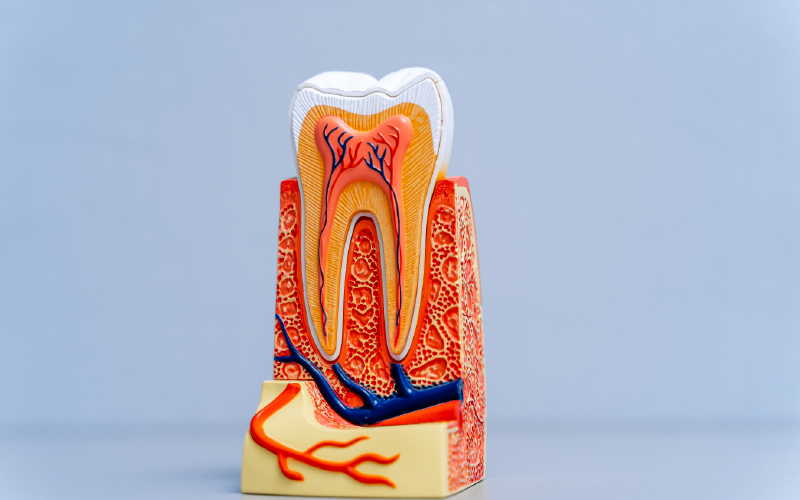
The dental pulp is the soft, growing tissue found in the center of a tooth. It is located within the pulp chamber and extends into the root canals, which are tiny channels that connect the pulp chamber to the roots of the tooth. The dental pulp contains a network of blood vessels, nerves, and connective tissue.
What Causes a Root Canal Infection?
A root canal infection, also known as pulpitis, occurs when bacteria enter the dental pulp, leading to inflammation and infection. The main causes of root canal infections include untreated tooth decay, dental trauma or injury, cracked or fractured teeth, gum disease, deep dental fillings, tooth grinding (bruxism), and dental abscesses. Prompt treatment is necessary to remove the infected pulp and save the tooth.
Signs You Should Consider a Root Canal
Several signs indicate that you should consider getting a root canal treatment. If you experience any of the following symptoms, it is essential to consult a dentist to determine if a root canal is necessary.
1. Persistent or Severe Toothache
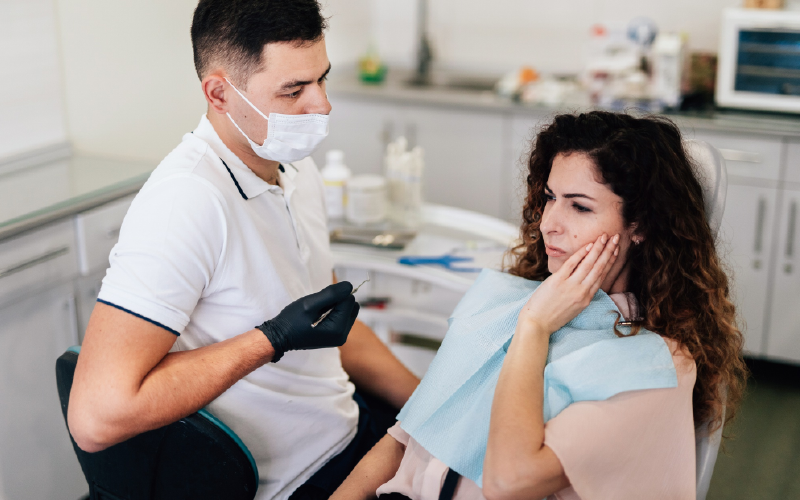
If you have a toothache that continues to persist or is particularly severe, even after taking over-the-counter pain relievers, it could be an indication of an infection in the dental pulp. The infected pulp needs to be removed through a root canal procedure.
2. Sensitivity to Hot or Cold
Increased sensitivity in a tooth, especially if it lingers after exposure to hot or cold temperatures, may be a sign of inflammation or infection in the dental pulp. This increased sensitivity develops because the injured pulp can no longer shield the nerve endings inside the tooth.
3. Swelling and Tenderness
Swelling and tenderness in the area surrounding a tooth may indicate an underlying infection. The body’s immune response to the infection can cause inflammation and the development of these symptoms.
4. Darkened Tooth

A tooth that has become noticeably darker or discolored compared to the surrounding teeth can be a sign of damage or infection within the dental pulp. The discoloration occurs when the blood vessels within the pulp are compromised.
5. Abscess Formation
An abscess is a pocket of pus that occurs at the base of a tooth due to a severe infection. If you notice a pimple-like bump on the gums near a tooth, it could be an indication of an abscess. Abscesses require immediate attention, often including a root canal treatment to eliminate the infection.
6. Painful Sensation When Chewing
If you experience pain or discomfort when biting or chewing, it could indicate an infected tooth. The pressure applied during chewing can aggravate the already compromised dental pulp and cause pain.
7. Cracked or Fractured Tooth
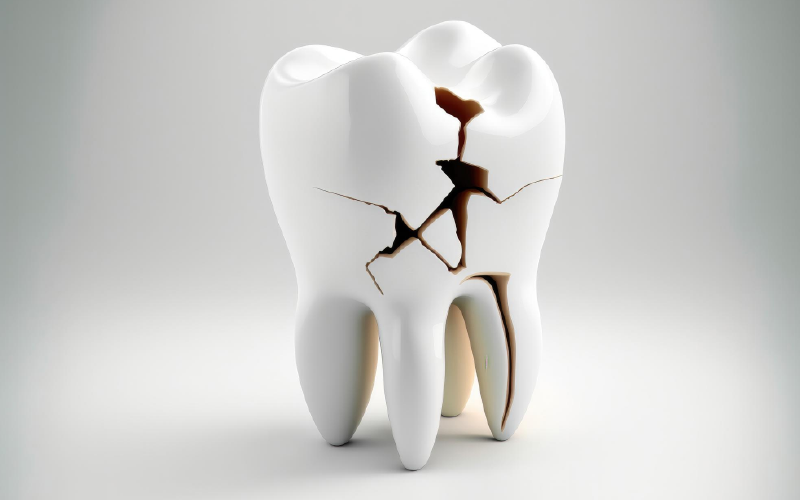
A tooth that is cracked or fractured can provide an entry point for bacteria to reach the dental pulp, leading to infection and inflammation. In such cases, a root canal may be necessary to remove the infected pulp and restore the tooth.
8. Lingering Pain After Dental Procedures
If you have recently undergone dental procedures on a tooth and continue to experience prolonged sensitivity or pain, it may suggest that the dental pulp has been irritated or infected. A root canal might be needed to address the underlying issue.
9. Gum Recession or Pus Discharge
Gum recession, where the gum tissue pulls back from the tooth, or the presence of pus or discharge around a specific tooth can be a sign of a dental problem, potentially requiring a root canal. These symptoms often indicate an infection that has spread from the dental pulp to the surrounding tissues.
Read Also: Essential Tips to Prevent Dry Socket After Tooth Extraction
What Is Root Canal Surgery?
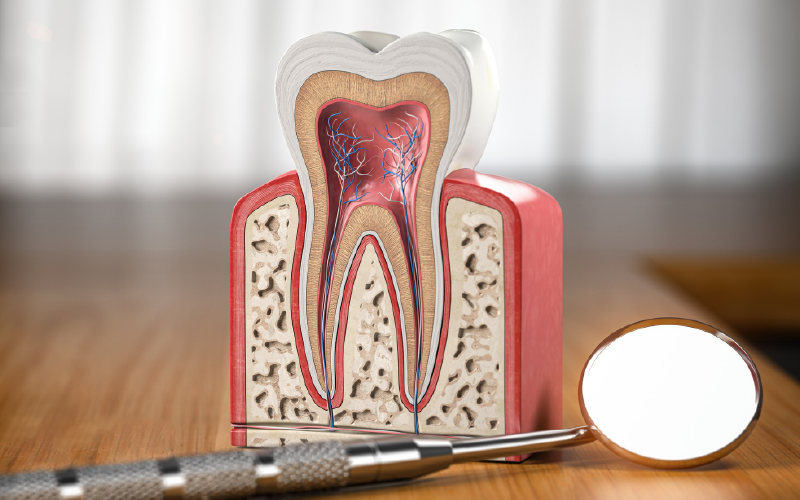
Root canal surgery, also known as apicoectomy or root-end resection, is a surgical procedure performed when a conventional root canal treatment has been unsuccessful or when there are specific complications that cannot be addressed through non-surgical means. It is a minor surgical procedure aimed at treating infections or persistent problems in the root tip (apex) of a tooth.
Here’s an overview of the root canal surgery process:
1. Evaluation and Preparation
Before the surgery, the dentist or endodontist will examine your tooth, review your X-rays, and determine if root canal surgery is the appropriate treatment option. Local anesthesia is used to assure your comfort during the treatment.
2. Accessing the Root Tip
In order to reveal the underlying bone and root tip, an incision is made in the gum tissue near the afflicted tooth.The dentist will carefully remove any infected or inflamed tissue from the end of the root.
3. Removal of the Root Tip
Using specialized instruments, the dentist will remove the infected or damaged portion of the root tip. This may involve resecting a small portion of the root, as well as any surrounding infected tissue.
4. Cleaning and Sealing
The root canal is thoroughly cleaned and disinfected to remove any remaining infection. The dentist may place a small filling material, such as gutta-percha, to seal the end of the root and prevent further infection.
5. Suturing and Healing
The gum tissue is sutured back into place, allowing the area to heal properly. The sutures are typically dissolvable and will naturally dissolve over time.
6. Post-Surgical Care
You will receive instructions on post-surgical care, including guidelines for oral hygiene, pain management, and any necessary follow-up visits. It’s crucial to follow these instructions for optimal healing and recovery.
Read Also: The Benefits of Professional Teeth Whitening
How long does a root canal treatment take?
Recovery time after a root canal varies, but most individuals can expect to recover within a few days to a week. Mild discomfort or sensitivity may occur during this time, but it can be managed with over-the-counter pain relievers.
Following post-operative instructions and attending follow-up appointments is important for a smooth recovery. Contact your dentist if you have concerns or experience severe or prolonged pain.
How Much Does a Root Canal Cost
In general, root canal treatment tends to be more expensive than a routine dental filling due to the complexity and time required for the procedure.
It typically involves multiple steps, including examination, X-rays, anaesthesia, removal of infected pulp, cleaning and shaping of root canals, filling the canals, and potential restoration with a dental crown or filling.
A single-tooth root canal operation might cost between $500 and $1500 in the United States.
Conclusion
In conclusion, root canal surgery is a specialized dental procedure performed when a standard root canal treatment is insufficient to save a tooth with a persistent infection or other complications. It may involve procedures such as apicoectomy, root resection, or intentional replantation.
At Knfdds, we specialize in providing affordable dentistry in Colorado, including advanced procedures like root canal surgery, ensuring our patients receive high-quality care without breaking the bank.
For best dentist in littleton co, it is important to consult with local dentists or endodontists who can provide appropriate evaluations, and treatment options, and perform root canal surgery if necessary.

